Feature Article: The MEG and how it is used with patients who have medically resistant epilepsy
What is Magnetoencephalography (MEG)?
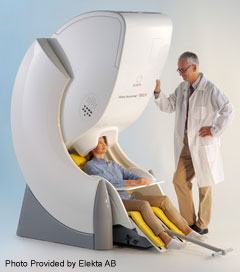
MEG is cutting edge technology used for mapping brain function. It is a non-invasive test that uses over 300 highly sensitive sensors that detect magnetic fields that are produced from the electrical activity of the brain. It is a completely painless test and uses no injections or radioactivity.
In What types of conditions would MEG be used for?
Magnetoencephalography is approved for use in two different patient populations: epilepsy patients and tumor/brain lesion patients. In both cases, the test is used as part of a pre-surgical evaluation.
In epilepsy, certain areas of the brain generate abnormal electrical signals, which create magnetic fields. The MEG records these abnormal magnetic signals and through sophisticated technology and software it can help determine where the abnormal electrical activity is coming from in the brain with remarkable accuracy. The results of the MEG are combined with a high resolution MRI and reconstructed into a 3-D image.
The same principles are in play when the MEG is used to localize certain types of critical brain function prior to surgery in patients with brain tumors or other brain lesions. Areas of brain function that the MEG can detect include motor, sensory, visual, auditory, and in some cases speech. Patients are asked to perform tasks or detect signals to test that brain function. When they do that an electrical signal called an evoked potential is generated in the brain’s cortex. This evoked potential also generates a magnetic field, which is what the MEG detects. Surgeons use this information to avoid operating in and around the area of critical brain function to avoid a post-operative neurologic problem.
What is a patient asked to do during functional brain mapping?
To test the auditory area a patient is asked to put in earplugs and listen to a series sounds. To test sensory areas a slight electrical stimulation is given to one of the nerves in the wrist or ankle. For motor testing a patient is asked to do a repetitive movement, such as tap your finger. Speech and language are tested in various ways.
How is MEG different than an MRI and EEG?
An MRI is a diagnostic test that assesses details of brain structure. Neurologists and neurosurgeons order a brain MRI scan to view the structure of the brain and assess for abnormalities such as strokes, hemorrhages, vascular abnormalities, tumors, scars, an abnormal growth and development patterns and so on. An MRI is an imaging study and is in essence a photograph or snapshot of the brain (or other body area) at a given instant in time. An EEG is a physiologic test. It assesses brain cell activity as opposed to brain structure. Abnormalities on an EEG may imply that something is wrong with brain cell function, but may not tell us exactly what. Specific EEG abnormalities, like epileptiform discharges can help establish a diagnosis of epilepsy, but still do not tell us the cause. EEG and MRI are complimentary in that regard.
Likewise EEG and MEG are complimentary. EEG detects electrical signals from the brain – normal and abnormal – and based on the orientation of the electric signals, generates a waveform, which is read and interpreted by trained electroencephalographers. Electrical signals can have different orientations (directions). An EEG generates waveforms and analyzes radially oriented signals better. The MEG also generates waveforms; they are generated only when electrical signals tangentially oriented. Therefore, both MEG and EEG can provide complimentary information about the electrical activity of the brain. A major difference between MEG and EEG is how the devices are influenced by normal and abnormal anatomy. While EEG (i.e. electrical) signals are influenced by various aspects of anatomy, including scalp and bone, and are even distorted if a patient has had previous brain surgery, magnetic signals are not. MEG, therefore, can be a better localizing tool for epilepsy patients who have had any form of brain surgery.
Does everyone with epilepsy need an MEG?
At this time MEG is approved to be used as part of a non-invasive pre-surgical evaluation for epilepsy surgery, and for pre-surgical brain mapping prior to neurosurgery. If a patient has epilepsy that is not responding to medicine, surgery may be an option. In selected cases, MEG can provide invaluable information on the location of the seizure focus and help guide an invasive evaluation.
Is there an age limit?
No, this is safe for all ages; in fact some research centers do fetal testing. The only real limitation is that the patient needs to hold still. This may be a challenge with small children, but a parent may be in the room to help calm them and hopefully get the child to sleep (ideal recording state).
How long does the test take?
A MEG is an outpatient procedure. The patient comes to the hospital and registers for the test. The actual testing takes 60-120 minutes, depending on how much data needs to be acquired. There is significant preparation before brain wave activity is detected: electrodes are applied and calibrated with precision – both EEG and MEG electrodes – the two diagnostic tests are run simultaneously. Electrodes are removed afterward. A patient may expect to spend at least a full morning or afternoon in the MEG center for the test.
How long does it take for the data to be interpreted?
Even in the simplest cases, it takes several hours for the data to be processed. Once processed, the magnetoencephalographer would take anywhere from 90 minutes to read and interpret a normal study to up to 5-6 hours to read and interpret a complicated study. Generating the report can also take a considerable amount of time.
Is a MEG covered by insurance?
For the clinical circumstances noted above, insurance companies will require a letter of medical necessity and once provided usually provide pre-authorization for the test.
What happens if there is no useful data from the MEG?
In some cases the MEG data is unremarkable. The reasons for this could vary. For example, a patient’s electrical activity is oriented such that the MEG can’t detect it. If that is the case we would expect to see EEG but not MEG activity. In those cases, we can still analyze the EEG data to provide localizing information. In some circumstances, no inter-seizure activity is recorded. In those cases, we would expect to see neither EEG nor MEG activity. As the MEG data is often thought to be critical in the surgical planning by the requesting physician, we may need to repeat the study at another time.
What happens if the patient has a seizure during the MEG?
The MEG is based on the localization of magnetic fields generated from spikes that occur in between seizures. Occasionally, a patient may have a seizure during the MEG, either with or without associated inter-seizure activity. Depending on the seizure pattern and characteristics, we may be able to localize the seizure onset and spread (of both MEG and EEG signals) and provide useful information to the referring team. If there is also inter-seizure data, the results may be particularly helpful.
What if the MEG shows that there is more than one area of the brain involved?
This type of result would have to be carefully interpreted by the referring team and considered along with the clinical information to determine if the patient is still a good surgical candidate.
Once the MEG and all of the other diagnostic tests are completed, when does the actual process of epilepsy surgery begin?
Once tests are complete, the treating team will hold a conference on the usefulness and meaning of the tests. If a patient is thought to be a good surgical candidate, the patient will be scheduled to meet the surgeon and go over the surgical plan.
